In my years of helping children with autism, I have heard many times (erroneously) that there is no science behind diet for autism, or the gluten-free casein-free diet (GFCF diet) for autism.
This is simply not true. There is a great deal of research illustrating why gluten and dairy can cause and contribute to symptoms and the condition of an autism spectrum disorder, and how a GFCF diet can help.
On one of my live Q&A calls recently, a wonderful medical doctor earnestly asked about what research existed on a gluten-free, casein-free diet for autism. While I’ve been writing and speaking on it for years, this request sparked my desire to put together the LATEST science to help fellow practitioners looking for science-based support for using the GFCF diet in your practice.
In this article, I will share 7 underlying biochemical mechanisms for which gluten and casein cause problems in autism, and studies showing how a GFCF diet helps, including one I was part of.
Recommending and helping your clients implement a gluten-free and casein-free diet for their child with autism (or themselves) can be beneficial in many ways, even life changing. I’ve seen children:
- Improve language skills and communication
- Reduce hyperactivity and increase focus and attention
- Improve eye contact
- Reduce anxiety and increase calm
- Improve socialization
- Reduce irritability and aggression
- Decrease digestive symptoms
- Improve sleep
You may have your own “success stories” from families in your practice and may know firsthand how beneficial the diet can be (I’d love to hear them in the comments below).
While this research is on autism, you’ll notice that the underlying factors apply to many other conditions including ADHD, anxiety, neurological conditions, digestive disorders, autoimmune conditions, and more.
Gluten and Casein
Gluten is a protein found in wheat, barley, rye, and triticale, and products made from them. The actual problematic component of gluten is called gliadin. But most often you’ll hear it referred to as simply gluten.
“Glu-ten” acts as a “glue” and helps flour-based foods maintain their shape. You can find gluten in many types of foods, such as pasta, soups, cereals, baked goods, even in dressings, sauces, and processed meats.
Casein is a protein in milk. While there are different types of casein in different animal milks (a conversation for another day), a casein-free diet avoids all milk and dairy products from all animals.
Some practitioners personalize their client’s diet plan with special milk products like camel milk or ghee once they see how their client does 100% casein-free. However, to really know how a casein-free diet works for a client, I always recommend to the practitioners in my BioIndividual Nutrition® Pediatric Program to remove all animal milk of any kind.
We will discuss the challenges related to gluten and casein and how they impact autism symptoms in depth later in this article.
Soy
Soy is also important to remove on a GFCF diet.
Soy has many of the same characteristics and effects as gluten and casein. Soy is one of the most common food sensitivities and is inflammatory. Soy can also form opioid compounds like gluten and casein.
So, when I’m working with clients or educating practitioners, I recommend removing soy as well.
To me, a GFCF diet is really a GFCFSF diet.
Personalized Autism Diet Plan
A personalized, BioIndividual Nutrition approach is one that is focused on the unique needs of the individual, and while a gluten-free casein-free diet is not the only “autism diet” out there, it is one of the most widely used and effective diets.
As a nutrition practitioner or health professional, you are likely aware that the body and brain are intricately connected. Autism is a whole body disorder. So for your clients, following a therapeutic diet plan based on their unique needs can reduce, or in some cases even alleviate, both their autism symptoms, as well as the physical symptoms and comorbid conditions like diarrhea, constipation, sleeping challenges, and skin rashes. While these are not part of an autism diagnosis, these physical symptoms are common in autism because of the underlying biochemistry that affects both body and brain.. As you improve the body, you improve the brain.
The result is healing that brings improved health, learning, mood, and behavior.
I use many diets in my nutrition practice for children with autism; however, the most common is gluten-free casein-free because I find it extremely helpful and fairly easy to implement. Given the prevalence of negative reactions associated with both gluten and dairy (in the autism and general population as well), it’s often the first therapeutic diet I suggest to people when getting started.
If your client needs more help you may want to consider a grain-free diet such as the Specific Carbohydrate Diet, GAPS diet, or Paleo. And I always recommend understanding how a low salicylate diet or low amine diet can improve behavior and mood. And other diets that I teach to practitioners in my BioIndividual Nutrition Pediatric Program include the low oxalate diet, low FODMAPs diet, low glutamate diet, ketogenic diet, and more.
A Safe and Effective Intervention
A question I get from both clients and practitioners is “Is a gluten-free and casein-free diet safe to implement?”
I have found that improving the nutritional density of foods, removing harmful additives and things devoid of nutritional value, and tailoring a diet to the unique needs of the individual has virtually no downside.
Additionally, eating foods that cause inflammation, like gluten and dairy, cause nutrients to not be able to be absorbed and cause deficiencies. So when someone says, “children ‘need’ dairy for the nutritional value,” I would argue that they do not, and that it can actually harm nutrient status.
On the other hand, it is important that we help clients eat a nutritious diet and meet their nutritional needs through foods and added supplementation when required.
I want to share a video from my friend and colleague Dr. James Adams, PhD on nutritional intervention and our published study.
Meal Planning On An Autism Diet?
A healthy gluten-free and casein-free diet includes foods such as: red meat, chicken, eggs, vegetables, fruits, nuts, seeds, potatoes, rice, and beans. There is a wide variety when it comes to naturally gluten-free and casein-free foods available. But, your clients may need coaching, meal ideas, and food lists to understand just how varied a diet they can have until they get the hang of it.
Another important piece of education your clients will need is to understand food labels and hidden sources of gluten and casein. Identifying hidden sources of these inflammatory and problematic foods goes a long way in getting your clients the results they are seeking.
Providing your client handouts to guide them with dietary implementation is important. My BioIndividual Nutrition Pediatric Program includes many handouts and guides that can be given to your clients related to this and other nutritional education. Whether you make your own or have access to already done-for-you handouts like mine, equipping your clients with tools is important to their success… and yours.
The Science and Research on How Gluten and Casein Negatively Affect Autism
As we move into the science behind the gluten-free and casein-free diet for autism, please pay particular attention to the issue of inflammation. This applies to both the gut and the brain. Localized inflammation in the gut can impact digestion and nutrient absorption, and gastrointestinal inflammation can become systemic causing inflammation in the brain. Neurological inflammation has been linked to many chronic conditions and diseases such as autism, ADHD, depression, anxiety, and more.
Reducing inflammation is critical for our clients to heal. Therapeutic diet intervention targeted to their personalized nutrition needs is a key to reducing inflammation, and the GFCF diet is a great place to start.
Opiates from Gluten and Casein Impact the Brain in Autism
Certain long-chain peptides have a very similar structure to natural opioid-binding peptides. Gluten and casein are two of these proteins. Gliadorphin (also known as gluteomorphin) is the name of the opiate peptide formed during the incomplete or partial digestion of gluten, and casomorphin is the opiate peptide derived from dairy.
There can be a few reasons as to why these peptides enter the bloodstream. Firstly, the body requires adequate enzymes to break down these proteins effectively. Specifically the DPP-IV enzyme is required. It has been shown that children with autism have lower DPP-IV activity. [1]
Leaky gut, a condition you may be very familiar with already, is another way these peptides can get into the bloodstream. Leaky gut, a condition where the intestinal lining becomes permeable, is common in autism. [2] When these peptides get into the bloodstream, they can bind to opiate receptors in the brain, causing issues like high pain tolerance or a feeling of being disconnected or “foggy”. Many clients report that their child self-selects foods with gluten and/or dairy, often at the exclusion of other foods because of this opiate connection. Removing gluten and/or dairy can then result in withdrawal symptoms in the beginning. However, after removal of these foods from the body, some families report an improvement in restrictive eating!
Additional research on how opioids in foods impact individuals with autism:
- This study postulated that the opioids from gluten and casein excreted in the urine are possible etiological factors, and the diet a treatment option, in autism. And researchers stated, “A gut-to-brain axis is both possible and probable” [3]
- Studies have linked A1 beta-casein (BCM-7) from certain forms of dairy with autism and schizophrenia [4]
- Gluteomorphins and casomorphins are found in the urine of people with autism [5]
- Studies show gluteomorphin/gliadorphin and casomorphin can impact neurotransmitters in the central nervous system resulting in the social impairment seen in autism [6]
Another consideration related to opioids is the inflammation they cause in both the gut and brain. Their direct impact on the brain can cause issues such as irritability, pain, anxiety, foggy thinking, as well as addiction to foods with gluten and dairy.
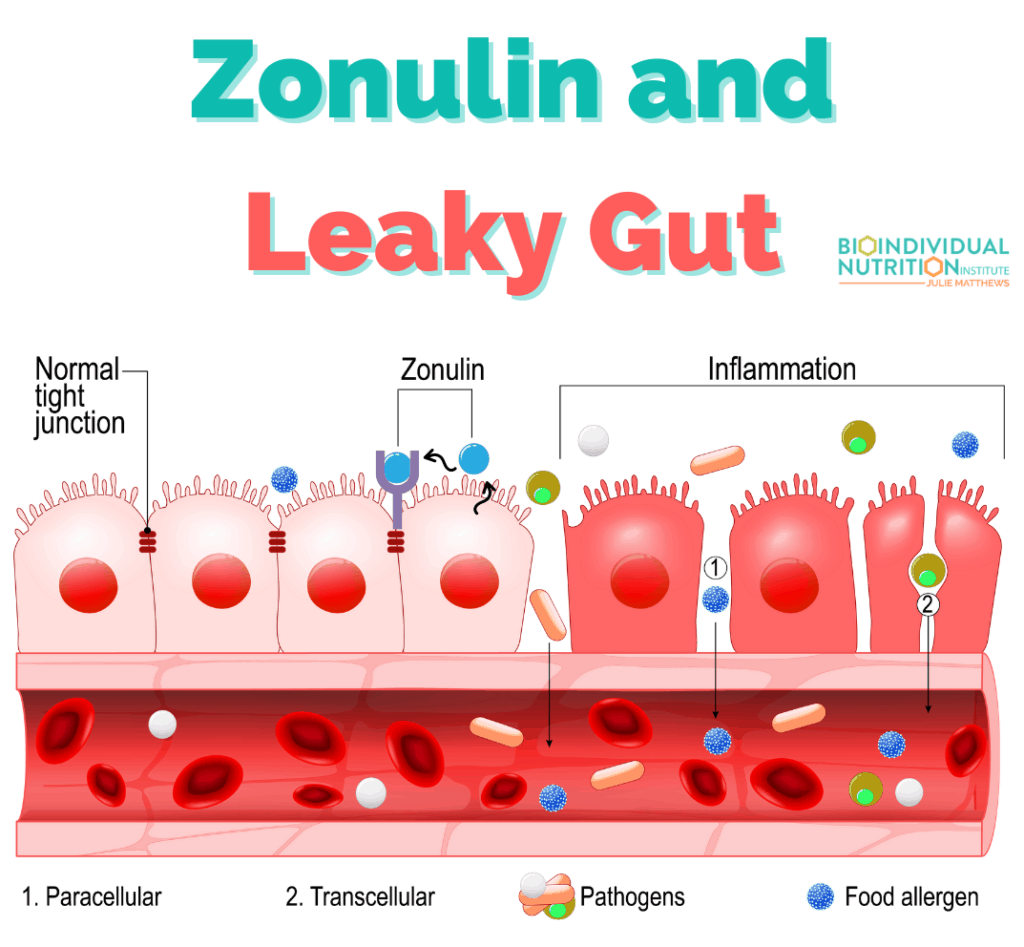
The Role of Zonulin in Leaky Gut and Autism Spectrum Disorders
Gluten is known to trigger a protein called zonulin so that is an additional advantage of a gluten-free diet. What is so problematic with zonulin is that it modulates the permeability of the GI tract in humans. It has been shown to “unzip” the tight junctions causing leaky gut. Scientific research has shown zonulin’s link to gut permeability in autism [7, 8] and other chronic inflammatory disorders including cancer, neuroinflammation, autoimmune disorders, and metabolic issues. [9]
Gut permeability can cause higher reactions to other food components for children with autism. As a result, your clients may see an increase in trouble concentrating, inflammation, diarrhea, constipation, and of course food allergies/intolerances. The brain cannot function optimally if the gut is unhealthy because of the gut-brain connection.
Individuals with ASD have a higher prevalence of gastrointestinal distress (read my article on NourishingHope.com). Additionally, the severity of GI symptoms has been linked to autism symptom severity in a study by Dr. James Adams. [10]
The study referenced above on zonulin from 2021 showed that children with severe autism had significantly higher serum zonulin than controls. This could be the missing link from Dr. Adams’ study in regards to the correlation between autism severity and GI severity! It may be related to increased permeability of the gut.
Children who follow a gluten-free diet have lower incidence of leaky gut than those children who do consume it.
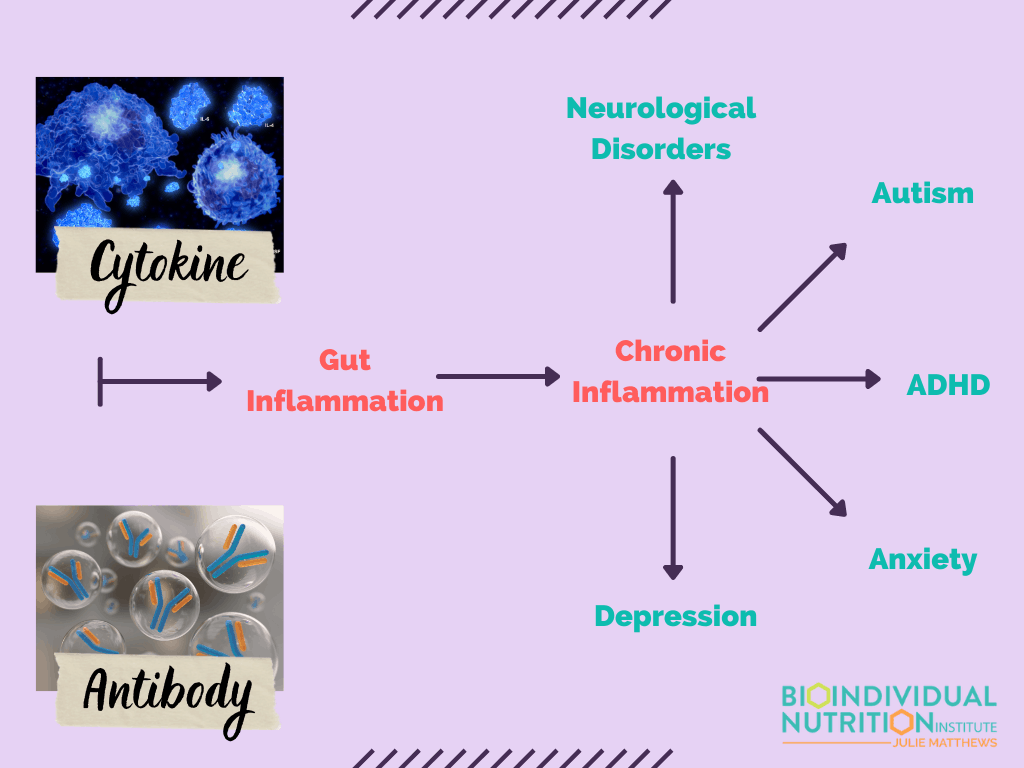
Inflammation in Autism Due to Gluten and Dairy
Inflammation can be created in the body and GI tract in response to IgG antibodies to foods. This issue is even more critical in the autism community. Researchers found high IgG antibodies levels to gliadin (i.e. gluten) in 87% of people with autism, as well as 86% of those with schizophrenia. They also found high IgG antibodies to casein in 90% of individuals with ASD and 93% in schizophrenia. [11]
Another study found elevated cytokines (inflammatory markers) to gluten in people with autism who had GI symptoms. [12]
This cycle of inflammation, issues in the gut, and symptoms such as constipation, diarrhea, gas, and pain can create systemic inflammation that also impacts the brain. In addition, the individual suffers because of incomplete breakdown of foods and poor nutrient absorption as well.
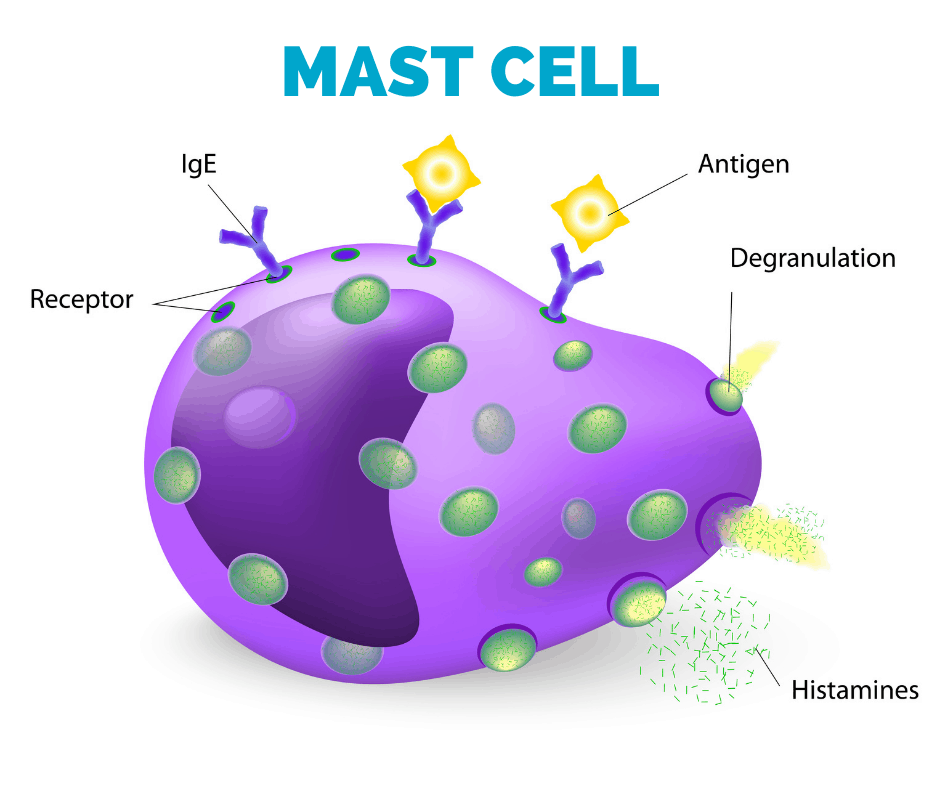
Histamine Released by Gluten and Casein and Mast Cell Activation in Autism
High histamine levels and mast cell activation are common in autism. And research even suggests that this activation leads to inflammation both in the brain and in the gut causing or exacerbating the symptoms of autism, and when exposed perinatally may even be a possible cause of the development of autism. [13]
Histamine release can be caused by general food allergies, as well as gluten and casein. [14] Gastrointestinal disorders can also be triggered by high histamine [15] along with resulting in high acid in the stomach and/or GERD. And in a converse manner, histamine can exacerbate food allergies.
Digestive disorders, high histamine, and mast cell activation in autism can lead to increased symptoms and severity of autism.
Higher risk of Celiac in Autism
Celiac disease is defined as an autoimmune response to gluten. This results in the body attacking the lining of the digestive tract, and causes severe digestive symptoms, along with other health conditions. While the majority of the time we see non-celiac gluten intolerance in autism, there is an increased risk of celiac disease as well.
In fact, there is research that shows people with autism are more likely to carry the HLA gene with the HLA-DRB1 *11-DQB1*07 structure, which raises the risks of celiac disease. [16]
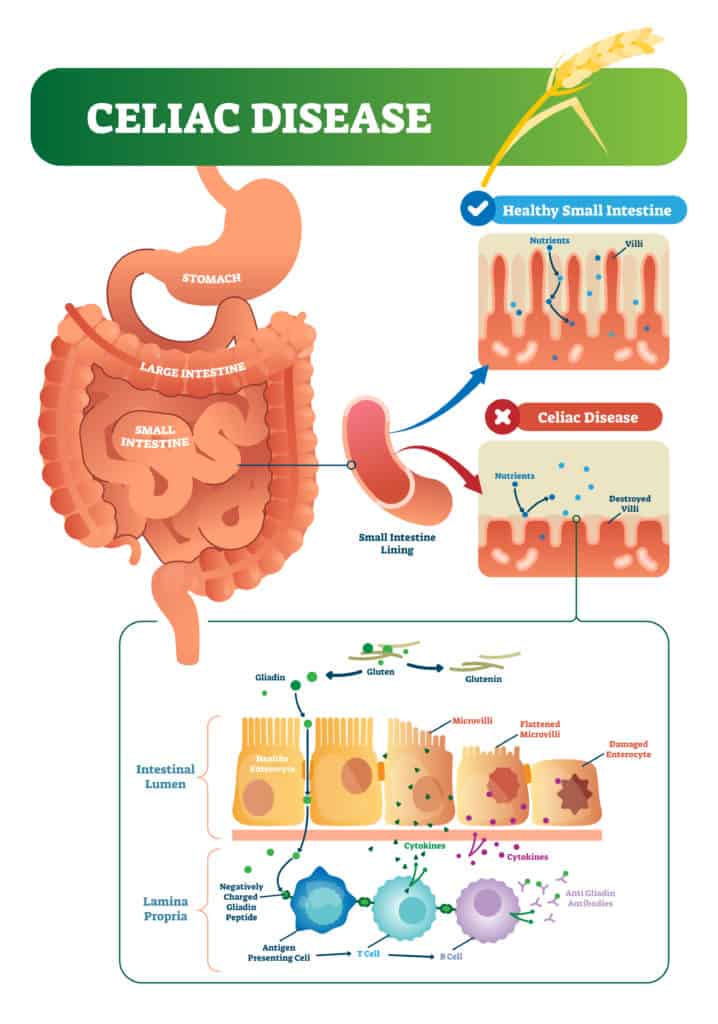
Celiac disease vector illustration. Labeled diagram with its structure. Autoimmune illness in stomach and intestine. Scheme with nutrients, healthy and destroyed villi.
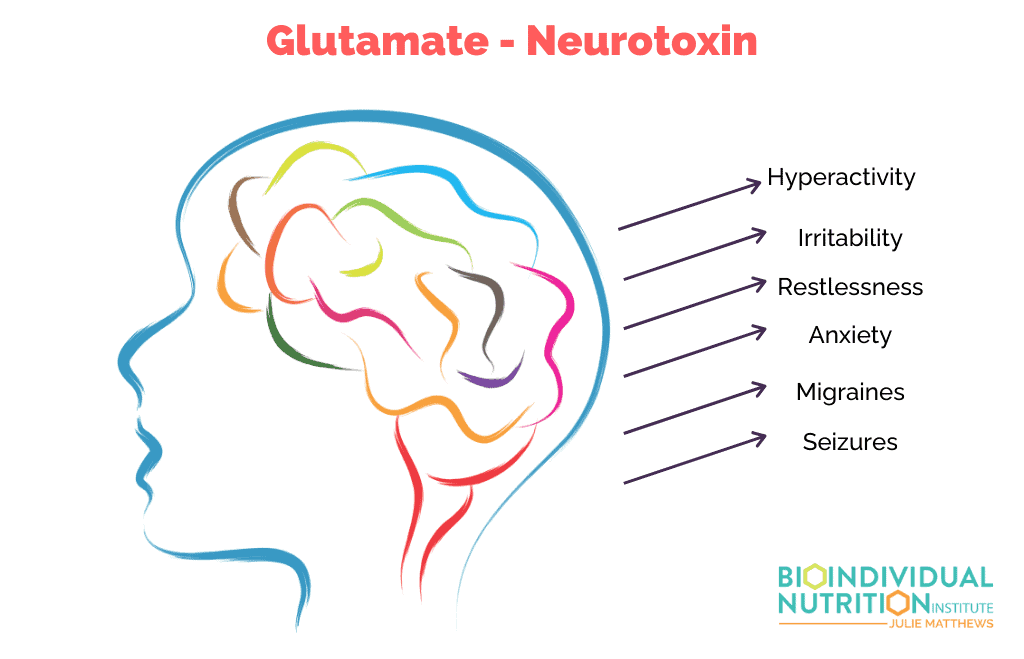
The Connection Between Gluten, Casein, and Glutamate in Autism
Studies show that individuals with autism have a higher risk of elevated glutamate. [17]
Some children and adults with autism are more sensitive to glutamate, an excitatory neurotransmitter. And they have less ability to convert glutamate to the calming neurotransmitter GABA. As a result, their brains are more responsive to the effects of glutamate and you can see increased hyperactivity, irritability, restlessness, anxiety, migraines, seizures, and many more symptoms in these individuals.
A diet rich in gluten and casein can increase glutamate levels because gluten is 25% glutamate by weight, and casein is 20%. For those sensitive individuals or those with high levels of glutamate such as those with autism, foods with gluten and dairy can worsen neurological symptoms, including stress, anxiety, irritability, and hyperactivity. Glutamate has also been shown to cause inflammation in the brain and gastrointestinal system. [18]
Reducing gluten and dairy in the diet can help reduce the symptoms of autism in some individuals, in part because of this glutamate connection.
Cerebral Folate Deficiency and Dairy
Cerebral folate deficiency involves folate not being able to be adequately transported into the brain because of autoantibodies to the folate receptor. This means the brain does not have adequate folate. Some children with autism have this condition. Cerebral folate deficiency can cause slow head growth, low muscle tone, irritability and sleep problems, loss of bodily movement, speech complications, and seizures.
There is scientific data showing that 75.3% of children with autism had autoantibodies to folate receptors. [19]
So for children with autism who have cerebral folate deficiency, studies show that soluble folate-binding proteins in milk cross react with folate receptors, this increases autoantibodies to folate receptors making the problem even worse by decreasing folate to the brain even further. But, the good news is that studies show removing dairy from the diet can reduce folate receptor autoimmunity in cerebral folate deficiency syndrome. [20]
Removing dairy from the diet reduces folate receptor autoantibodies and autoimmunity.
Scientific Research: Gluten-Free Casein-Free (GFCF) Diet Improves Autism Symptoms
Now that I have given you the underlying factors that can cause gluten and dairy to be problematic for individuals with autism, I want to also share the growing scientific data on the efficacy and benefits of removing gluten and casein from the diet.
Study Shows 91% of Children with Autism Had Improved Behavior, Speech, and/or GI Symptoms with GFCFSF
We’ve learned through the research that autism may be accompanied by inflammatory immune responses. This mechanism may also be what predisposes them to sensitivity to the proteins in wheat, dairy, and soy. Inflammation of the digestive system is the result of this increased sensitivity to these dietary proteins and this often exacerbates negative behaviors.
One very interesting study showed clinical improvement in 91% of the children as observed by therapists, teachers, and parents following the implementation of a gluten-free, casein-free and soy-free (GFCFSF) diet. Improvements were seen in speech, focus, sleep, GI symptoms, and less hyperactivity. [21]
6.7 points in Non-Verbal IQ and 4.5x Developmental Age Improvement from GFCFSF Diet and Nutrition Intervention in Autism
I am particularly proud of this next study because I was part of it! It showed a 6.7 pts increase in non-verbal IQ and a 4.5 fold developmental age improvement.
The study included individuals aged 3-58 years old who implemented a healthy gluten-free, casein-free, and soy-free diet, a multivitamin/mineral formula, an essential fatty acid supplement, carnitine supplementation, digestive enzymes, and epsom salt baths. You can read my complete write up here.
Major improvements outside of development and IQ included: a reduction in autism symptoms, decrease gastrointestinal symptoms, improved language, increased focus, reduced anxiety, and more. [22]
Increased Social and Communication Skills Along with Reduced Autism Behaviors with GFCF Diet
A review of the existing scientific literature found consistently positive results with a gluten-free and casein-free diet for autism. The literature included both individual case studies and papers where groups of children were studied.
What researchers found was an overall decrease in autism behaviors as well as increased social skills and communicative skills.
It is important to note that they found the autism traits reappeared after the diet was broken. [23]
Better Development for Individuals with Autism on a GFCF Diet
This study evaluated the effects of a gluten-free and casein-free diet for children with autism in regards to urinary opioid peptides associated with gluten, gliadin, and casein.
The study concluded that children following a gluten-free and casein-free diet had better development than the control group. [24]
Significant Improvement in Autism and ADHD Symptoms in Children with ASD on the GFCF Diet
In this two-stage, 24-month, randomized, controlled trial, 72 Danish children (ranging from 4 years old to 10 years 11 months) were assigned to diet (A) or non-diet (B) groups. To assess core autism behaviors they used the Autism Diagnostic Observation Schedule and the Gilliam Autism Rating Scale. Vineland Adaptive Behaviour Scales was used to determine developmental level, and the Attention-Deficit Hyperactivity Disorder – IV scale was used to determine inattention and hyperactivity.
There were significant improvement scores in the diet group on all of the scales by 12 months. Group B was also assigned to the diet midway through the trial because of the improvement seen in group A! The results indicated that dietary intervention using a gluten-free and casein-free diet may positively affect developmental outcomes for children with ASD. [25]